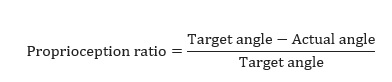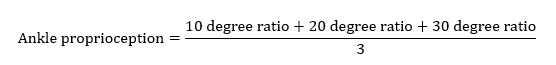Participants and Design
Participants were recruited from among inpatients at a rehabilitation hospital (National Rehabilitation Center, Seoul, South Korea) from January to May 2018. The eligibility criteria were as follows: (1) chronic post-stroke hemiparesis; (2) weakness of ankle muscles on the affected side (Medical Research Council Scale, ankle dorsiflexion (DF) strength range, grades 1–4); (3) Modified Ashworth Scale score <3 for spasticity in the affected ankle; (4) impaired light touch sensation on the plantar aspect of the head of the first metatarsal of the affected foot; and (5) Functional Ambulatory Category Score ≥3. Potential participants were excluded if they had complications of orthopedic disorders and cognitive impairment (Mini-Mental State Examination Score ≤24).
A double-blind, parallel-group, randomized controlled trial with blinding of assessors and concealed allocation was conducted. A person uninvolved in the trial created a blocked random allocation schedule for 35 participants using Microsoft Excel®, and participants were divided accordingly into the experimental or control groups after the baseline assessment to receive AMT-EST or only ES, respectively, on the affected ankle for 4 weeks. All participants were reassessed at the end of the 4-week intervention period.
Ankle Movement Training System
The ankle-training device used in this study was developed for intensive and selective training on the paretic ankle in stroke patients. The main feature of the ankle training device was to reproduce the actual biaxial ankle movement that was applied by a seesaw-type foot cradle that pivoted along the transverse ankle axis, and the foot force plate was rotated along a 42°-tilted subtalar axis relative to the foot cradle. The improvement in ankle PROM, stiffness, and walking performance on uneven surface as a result of passive biaxial ankle training using this ankle device in chronic stroke patients has been reported previously [15]. In this study, an ankle function enhancement training protocol that applied ES in accordance with passive biaxial ankle movement was constructed and applied (more information about the ankle training system in Supplement I of the online-only Supplemental Material).
Intervention
Experimental group
Before the training session, the participants were asked to comfortably sit on a height-adjustable chair with his/her knees flexed at 90°, to place his/her paretic foot on the footplate of the ankle-training device, and to place his/her non-paretic foot on the height-matched footrest. The paretic foot was fastened to the force plate in the foot cradle using three length-adjustable straps (Figure 1). The two electrode pairs (5×9 cm; RehaTrode, Hasomed, Germany) were placed over the common peroneal nerve as it passed over the head of fibula and the motor point of the tibialis anterior. Other electrode pairs were placed slightly lateral to this and targeted toward the peroneus longus (Figure 1). ES was applied to confirm that the location of the attached electrodes caused proper ankle DF (tibialis anterior) and EV (peroneus longus).
AMT-EST was performed for 4 weeks, with 5 sessions per week. All participants completed more than 90% of the training sessions. The duration of one training session was 40 minutes, which comprised a 5-minute warm-up, 30 minutes of ankle training, and a 5-minute cool-down. In the warm-up session, the PROM of ankle DF, plantarflexion (PF), INV, and EV were measured, and all ankle training was performed within 80% of the full ankle range of motion. Subsequently, the participants performed a PROM exercise for each ankle direction along either talocrural or subtalar joint. In the ankle-training session, the simple and combined ankle PROM exercise with ES was performed along the ankle (talocrural) and subtalar (talocalcaneal) axes. The simple movements consisted of 20 repetitions of DF-PF and INV-EV, and the combined movements consisted of 40 repetitions of inverted PF and everted DF (diagonal movements), which are more commonly used in actual movement. All ankle movement speed was slow, at 2.14°/s, to avoid ankle spasticity [15]. The timing of the starting and ending of the paretic ankle DF and EV movements was directly observed by the therapist who then applied ES (Microstim2, Medel GmbH, Germany) current with 0.28-ms pulses, at 35 Hz with pulse durations from 300 to 450 µs in alternating mode within the participants’ tolerance level, via surface electrodes. The amplitude was adjusted to produce muscle contractions without causing patient discomfort [20]. In the last cool-down, 10 simple PROM exercises were performed for each ankle direction (Figure 2).
Control group
Participants in the control group received ES on paretic ankle muscles for 4 weeks, with 5 sessions per week. The participants received PROM exercises by the ankle training device for the first 5 minutes (warm-up), ES on the paretic ankle for 30 minutes (training session), and then PROM exercise for the last 5 minutes (cool-down; Figure 2). The ES (Microstim2, Medel GmbH, Germany), with a pulse frequency of 35 Hz in alternating mode and pulse duration of 300−450 µs, was applied at the same position as the electrodes were applied in the experimental group in the sitting position.
Outcome Measures
The primary outcome was ankle function, including ankle proprioception, PROM, and strength. Proprioception was assessed by evaluating the joint position sense of the ankle DF, PF, INV, and EV using an ankle-training device with constant velocities (2.14°/s). Participants wore eye masks and earplugs in a sitting position with the other lower limbs fixed to allow only ankle movement. The assessment comprised two steps. In the first step, the ankle was moved passively from the initial angle (0°) to the randomly assigned 10 target angles (10°, 20°, and 30° of ankle PF and INV; 10° and 20° of ankle DF and EV; according to normal range of motion of the ankle), while asking the participant whether the ankle movement and the direction of movement were perceivable. After staying at the target position for 5 seconds, the ankle was returned to the initial angle. In the second step, the paretic ankle was moved toward the target angle again and the participant was asked to say “stop” when they felt that they had reached the target angle (actual angle). No feedback about results was provided to the participant during the task. The assessment began with a period of familiarization. Three ankle movements were evaluated per direction, and a total of 38 measurements including dummy trials (no movement) were performed. For statistical analyses, the proprioception ratio were calculated in relation to angular differences, which means that the difference between the target angle and actual angle was ascertained using the following equations [21]:
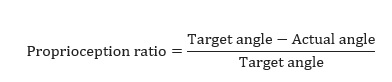
Finally, the proprioception ratio for all four directions (DF, PF, INV, and EV) was calculated as the average value of the proprioception ratio that was measured three times for each angle. The larger the proprioception ratio value, the greater is the deficit.
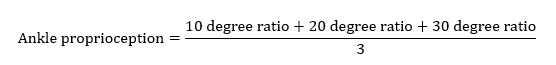
The PROM of the paretic ankle was measured using a portable goniometer by a skilled physiotherapist. The average values of three measurements of maximum PROM of DF, PF, EV, and INV were recorded. To measure ankle strength, the isometric contraction force of the paretic ankle muscle was measured using a portable manual muscle strength tester (Lafayette, USA, 2018). The isometric strength of the ankle dorsiflexor, plantar flexor, invertor, and evertor was measured for 5 seconds, and the maximum value was recorded.
The secondary outcomes included motor, balance, and gait function, evaluated by the Fugl–Meyer Assessment for the lower extremity (FM-L), Berg Balance Scale (BBS), the Timed Up and Go test (TUG), the Korean version of the Fall Efficacy Scale, and walking speed. A description of the assessment method is available in Supplement III of the online-only Supplemental Material.
Statistical Analyses
The sample size was calculated according to the study sample of a study that reported the effect of repeated passive exercises on the knee’s proprioception in patients with hemiplegia [22]. Calculations were performed with a paired t-test value of the knee position sense for a comparison of the before and after intervention values, using an alpha of 0.05 at 95% power. The total sample size was determined to be 6 for each group (effect size: 1.744, actual power: 0.975). The G * Power 3.1.9.2 program was used.
The normative distribution was assessed using the Shapiro–Wilk test. Some sample characterization data did not show normative distribution, and the Mann–Whitney U test or chi-squaretest was conducted for comparing the groups at baseline. Within each group, the Wilcoxon signed rank test was used to compare data from the pre- and post-intervention tests. To examine the main effects of the interventions, a 2 (group)×2 (time) ANOVA with repeated measures was performed. The relationships between ankle proprioception and clinical outcomes were examined using Spearman’s correlation coefficient (r). All statistical analyses were performed using SPSS ver. 22.0 (IBM, Armonk, NY, USA), and the significance level was set at P<0.05.